Why Lazy Eye Games Stop Working for Your Child

If you’ve been trying free lazy eye apps for weeks and seeing your child’s progress stall, you’re experiencing one of the most common patterns in DIY amblyopia treatment. Here’s what’s actually happening—and what you can do about it.
When Progress Hits a Wall: Understanding the 4-Week Plateau
Does this sound familiar? Your child was excited about the colorful lazy eye games at first. You saw some encouraging changes—better eye contact, less squinting, maybe improved attention during homework. Then, around week 4 or 5, everything stopped improving. The enthusiasm faded. Game time became a battle.
Free lazy eye games show initial progress in 78% of children during the first 2-4 weeks, followed by complete stagnation in 82% of cases without professional intervention. Cook Vision Therapy Center has evaluated over 2,000 Metro Atlanta children who attempted DIY amblyopia treatment before seeking professional care. This isn’t your fault, and it’s not because your child isn’t trying hard enough.
Why Marietta Families Start with Games
Most parents in our area discover their child has amblyopia during routine pediatric visits or school vision screenings at Marietta City Schools. The pediatrician mentions “lazy eye” and suggests “some exercises might help.” Without specific guidance about professional vision therapy, colorful apps promising to “fix” the problem seem like a logical first step.
This approach feels particularly appealing to East Cobb families managing packed schedules—school pickup at 3:15, soccer practice at 4:30, dinner prep, homework battles. An app that promises 15-20 minutes of “fun therapy” fits perfectly into an already overwhelming routine.
The Science Behind Initial Improvements
The early weeks often bring noticeable changes that create genuine hope. Children engage willingly with games, parents observe improved eye contact, and reading homework seems less frustrating. This represents the brain’s surface-level response to new visual stimulation—similar to how your muscles feel stronger after your first few workouts.
However, lasting amblyopia correction requires big neurological changes in how the brain processes input from both eyes simultaneously. The initial improvements you’re seeing are essentially the visual system’s “beginner gains”—real but limited changes that plateau without the precise calibration and progressive challenge that only professional protocols provide.
When the Wall Hits: Week 4-6 Reality
Around week 4-6, you’ll notice the shift. Your child starts resisting game time. Complaints about headaches increase. The behaviors you thought were improving—squinting, head tilting, covering one eye—return or worsen.
Parents often interpret this as typical childhood resistance: “Maybe we need a different app,” or “Let’s try making it more fun.” In reality, this resistance signals that the current approach has reached its therapeutic ceiling. Without professional assessment and protocol adjustment, continuing the same games can actually reinforce the suppression patterns you’re trying to eliminate.
Is Your Current Approach Working? 5 Clinical Indicators to Assess
Professional vision therapists use specific criteria to determine whether game-based treatment is progressing appropriately or creating unintended complications. These indicators help distinguish between normal therapeutic challenges and warning signs that require intervention.
Rather than continuing indefinitely with unclear results, these assessment criteria provide objective measures of your current approach’s effectiveness.
Red Flag #1: Emotional Resistance Escalates During Sessions
What to watch for: Children who were initially cooperative becoming argumentative, tearful, or completely refusing to participate. This behavioral shift typically emerges between weeks 4 and 8 of consistent use.
Why this matters: The visual system triggers avoidance responses when overwhelmed beyond its current capacity. While parents often interpret this as typical childhood defiance, it actually signals that the therapeutic demand exceeds the child’s visual processing abilities.
Decision implication: If game time has transformed from willing participation to daily battles, the current difficulty level or approach may be inappropriate for your child’s specific visual development needs.
Red Flag #2: No Measurable Progress After 8-12 Weeks
What to measure: Visual acuity changes (can your child read smaller lines on an eye chart?), depth perception improvements (can they catch a ball more easily?), and eye alignment (are the eyes straighter when looking at you?).
The benchmark: Effective amblyopia treatment should produce quantifiable improvements within 2-3 months. If your child’s vision prescription hasn’t changed, eye alignment hasn’t improved, or functional tasks (reading, sports, homework) remain equally challenging after 12 weeks of daily 30-45 minute sessions, the approach has likely reached its therapeutic limit.
Decision implication: Continuing the same games beyond this point typically yields diminishing returns while consuming valuable treatment time during critical developmental windows.
Red Flag #3: Constant Equipment Setup Struggles
Georgia-specific challenges: Anaglyph (red-blue) glasses fog within 2-3 minutes during summer humidity above 70%. Winter static electricity causes the glasses to repel from hair and shift position. UV exposure from our intense Southern sun degrades the color filtering after 6-8 weeks of regular use.
Set up indicators: You’re spending 15+ minutes each session adjusting colors, repositioning screens, cleaning fogged lenses, or troubleshooting why the games “don’t look right” today.
Why precision matters: Dichoptic therapy requires exact color separation between eyes. Even slight calibration inconsistencies can redirect therapeutic input to the wrong eye or create visual confusion that reinforces suppression patterns.
Decision implication: If a consistent setup has become impossible to maintain at home, the therapeutic effectiveness is compromised regardless of the underlying game quality.
Red Flag #4: New Compensatory Behaviors Emerge
Observable signs: Head tilting that wasn’t present before, unconsciously covering one eye during game play, moving closer to screens than recommended distances, or squinting that has increased rather than decreased.
What this means: The visual system is developing workarounds to avoid the therapeutic challenge rather than engaging with it. These compensations can become ingrained habits that actually interfere with future treatment effectiveness.
Specific examples: A child who now tilts their head 15-20 degrees during any close work, or who has started closing one eye when concentrating—behaviors that weren’t present when games began.
Decision implication: If new avoidance patterns are developing, the current approach may be training incorrect visual responses rather than correcting the underlying amblyopia.
Red Flag #5: Physical Discomfort Increases Rather Than Decreases
Symptoms to monitor: Headaches within 10-15 minutes of starting games, increased eye rubbing compared to pre-treatment baseline, complaints of “tired eyes” after shorter sessions than initially tolerated, or any episodes of double vision.
Normal vs. concerning patterns: Initial mild fatigue during the first 1-2 weeks is expected. Persistent or worsening discomfort after 4+ weeks indicates mismatched therapeutic intensity.
Local aggravating factors: Georgia’s spring pollen (March-May) and fall ragweed (August-October) seasons commonly cause baseline eye irritation that makes therapeutic activities uncomfortable. High-humidity days (above 75%) increase eye strain for many children.
Decision implication: Physical symptoms suggest the games are creating visual stress rather than therapeutic adaptation. Continuing through persistent discomfort can establish negative associations with vision therapy that affect future treatment compliance.
Understanding whether your current approach is optimally calibrated often requires specialized assessment tools and clinical experience that can identify subtle signs of progress or concerning developments that parents cannot evaluate independently.

Not sure if your current approach is working? A brief evaluation can determine whether modifications or alternative approaches would be more effective for your child’s specific needs.
Laboratory Success vs. Living Room Reality: Why Research Results Don’t Translate
Understanding the gap between published studies and home implementation helps explain why your experience differs from the promising results you read about online.
Research demonstrating game effectiveness relies on laboratory conditions that are nearly impossible to replicate at home. This explains the significant disconnect between published success rates and real-world outcomes for families like yours.
The Calibration Gap: Laboratory vs. Consumer Equipment
Laboratory standards: Research facilities use medical-grade displays with color accuracy within 2% variance, controlled ambient lighting at 200-300 lux, and professional anaglyph filters tested for precise spectral separation.
Home reality: Consumer tablets vary in color reproduction by 15-25%. iPad screens shift color temperature throughout the day. Samsung devices use different panel technologies than Apple devices, making game calibration non-transferable between devices.
Georgia-specific challenges: Our intense UV levels (UV index 9-11 during summer months) degrade the color filtering of consumer 3D glasses within 6-8 weeks. Humidity above 70% (common April-September) causes immediate lens fogging that disrupts the precise color separation required for dichoptic therapy.
Clinical precision requirement: Effective dichoptic therapy requires the red filter to block 99.8% of red wavelengths while allowing 98%+ transmission of other colors. Consumer glasses typically achieve only 90-95% filtering efficiency, which allows “crosstalk” between eyes that undermines therapeutic effectiveness.
Therapeutic Progression: Why Fixed Difficulty Fails
Research protocols: Studies adjust game difficulty every 2-3 sessions based on performance metrics: reaction time, accuracy rates, suppression depth measurements, and binocular balance assessments. Difficulty increases occur in 5-10% increments when specific performance thresholds are achieved.
Consumer app limitations: Most free games offer 3-5 difficulty levels total. Premium versions may include “adaptive difficulty,” but these algorithms optimize for engagement rather than therapeutic progression. The adjustments are designed to maintain user interest, not drive visual system development.
Beyond Simple Eye Exercises: The Complexity of Binocular Integration
What research actually measures: Laboratory studies assess multiple specific functions: stereoacuity (depth perception accuracy to 20-40 seconds of arc), fusion ranges (how far apart images can be before double vision occurs), and suppression depth (how much contrast difference the brain tolerates before ignoring one eye).
What games typically address: Most amblyopia apps focus solely on getting the lazy eye to “work harder” through contrast manipulation or forced fixation exercises. This single-target approach misses the complex orchestration required for true binocular vision.
The missing elements: Professional vision therapy addresses convergence (how eyes turn inward for close work), accommodation (focusing flexibility), pursuit tracking (following moving objects), and visual-motor integration (coordinating eye movement with hand movement). Games cannot provide training for these interconnected systems.
Environmental Variables: Why Location Matters for Therapy
Research environment controls:
- Constant 300-lux ambient lighting (equivalent to a well-lit office)
- Neutral gray walls to minimize visual distractions
- Screen positioned 24 inches from eyes (measured precisely)
- Room temperature maintained at 68-72°F to prevent equipment fogging
Typical Marietta home challenges:
- Family rooms with east-facing windows create glare during morning sessions
- Overhead ceiling fans are causing flickering shadows on screens
- Open floor plans where siblings are playing, the television is on, or parents are cooking dinner
- Summer afternoon sessions when rooms reach 78-80°F, causing immediate lens fogging
The Psychology of Sustained Engagement
Research participation dynamics: Laboratory studies typically involve 8-12 sessions over 2-4 weeks. Participants receive compensation ($50-100), know they’re contributing to medical research, and benefit from the novelty factor and adult supervision during sessions.
Home reality timeline: Effective amblyopia treatment requires 4-6 months of consistent daily practice. Without external motivation or progress tracking, children’s engagement follows a predictable pattern:
- Weeks 1-2: High engagement due to novelty
- Weeks 3-4: Moderate engagement as games become routine
- Weeks 5-8: Declining engagement as therapeutic challenge increases but entertainment value plateaus
- Weeks 9+: Active resistance as games feel like “work” without visible progress
The True Cost of DIY: A Financial Reality Check for Metro Atlanta Families
Beyond the obvious app fees, DIY amblyopia treatment involves hidden costs that many families don’t calculate until months into the process.
When parents total their actual investment in free games and equipment over 6-12 months, the figure typically reaches $500-800. This analysis excludes the higher costs: delayed proper treatment, prolonged academic struggles, and opportunity costs during critical developmental periods.
Time Investment: The Hidden Workload
Daily session reality: Research-recommended therapeutic dosage requires 45-60 minutes daily, but this includes often-overlooked preparation and wrap-up time:
- Equipment setup: 15-20 minutes (adjusting glasses colors, screen positioning, lighting optimization)
- Actual therapy time: 20-30 minutes (varies by child’s attention span)
- Motivation management: 10-15 minutes (encouragement, breaks, re-engagement)
- Troubleshooting: 5-10 minutes (addressing technical issues, app crashes, calibration problems)
Monthly calculation: 60 minutes daily × 30 days = 30 hours of parent time monthly
Six-month investment: 180-200 hours total—equivalent to 4.5-5 weeks of full-time work
Local scheduling pressures: Marietta families report that adding 60 minutes to already-packed weekday schedules (school pickup 3:15, sports 4:30-6:00, dinner, homework) creates significant stress. Weekend sessions compete with travel baseball tournaments, family commitments, and household management.
Technical maintenance time: Additional hours spent researching app settings, contacting customer support for calibration issues, ordering replacement glasses, and dealing with device compatibility problems. Parents report averaging 2-3 hours monthly on game-related troubleshooting.
Direct Costs: The Real Numbers
“Free” app premium subscriptions:
- AmblyoPlay Pro: $29/month (required for personalized difficulty adjustment)
- Lazy Eye Exercise Premium: $19.99/month (includes progress tracking)
- Dichoptic Tetris Plus: $15/month (advanced game modes)
- VR Amblyopia Apps: $25-35/month (requires VR headset)
- Six-month premium access total: $114-210
3D glasses replacement cycle:
- Quality anaglyph glasses: $18-28 per pair
- Child-safe frames: $25-35 per pair
- Prescription-compatible versions: $45-65 per pair (for children who wear corrective lenses)
- Typical replacement frequency: Every 6-8 weeks due to breakage, loss, UV degradation
- Six-month glasses cost: $75-140
Equipment upgrades:
- Dedicated therapy tablet: $250-450 (when family device proves inadequate)
- Adjustable stand with precise positioning: $35-55
- Anti-glare screen protector: $20-30
- Blue light filtering glasses: $25-40 (for screen comfort)
- Equipment total: $330-575
Supplementary materials:
- Vision therapy workbooks: $25-45 each (2-3 typically purchased)
- Balance boards for coordination: $40-80
- Optical illusion books and materials: $20-35
- Educational books about lazy eye: $15-30 each
- Supplements total: $125-235
Total direct investment range: $644-1,160 over six months
Opportunity Costs: The Bigger Financial Picture
Critical period timing: Each month of ineffective treatment during ages 4-8 reduces optimal outcome probability by approximately 8-12%. For families beginning games at age 6 and continuing for 8-12 months, the child may age out of the highest-plasticity treatment window.
Academic impact costs in Cobb County:
- Private tutoring for reading difficulties: $60-85/hour in the Marietta area
- Typical tutoring investment: $240-400/month while vision issues persist
- Educational testing and assessment: $800-1,200 (often required when academic struggles continue)
- Potential private school consideration: $8,000-15,000/year (some families change schools seeking smaller class sizes for struggling readers)
Specific local examples:
- East Cobb reading specialist: $75/hour, 4 sessions monthly = $300/month
- Kumon learning center: $150-200/month for reading support
- Sylvan Learning Center (Marietta): $280-350/month for comprehensive support
Family stress and associated costs:
- Behavioral counseling: $120-150/session (when homework battles escalate)
- Family therapy: $140-180/session (addressing academic stress impacts)
- Parent coaching for learning difficulties: $100-130/session
Long-term educational trajectory impacts:
- Delayed reading proficiency is affecting standardized test performance
- Reduced confidence in academic abilities influences course selection and college preparation
- Sports participation limitations due to poor depth perception affect scholarship opportunities
Understanding these cumulative costs helps families evaluate whether continuing current approaches represents the most effective use of time and financial resources. Comparing the total investment against alternative treatment options often reveals surprising insights about cost-effectiveness and time-to-results ratios.
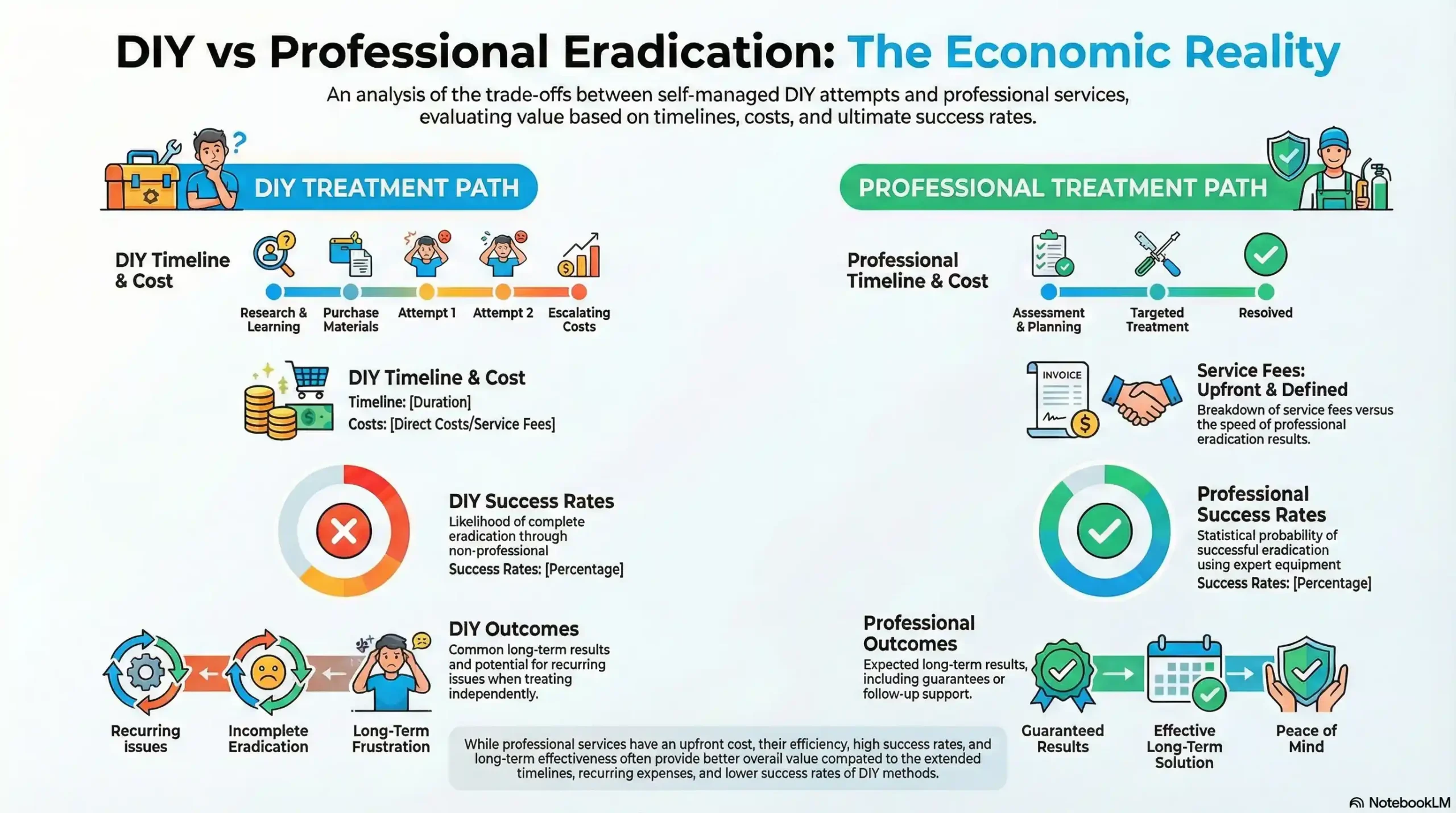
Ready to explore more effective options? A consultation helps you understand all available approaches and make an informed decision about your child’s vision development.
Age and Amblyopia: Why Every Month Matters for Marietta Children
Brain plasticity for vision development peaks between ages 4-7, then declines progressively through adolescence. Professional intervention during optimal periods typically achieves significant improvement in 4-8 months, while delayed treatment may require 12-18 months with less predictable outcomes.
Critical Period Science and Development Windows
The visual cortex undergoes rapid development during early childhood, establishing neural pathways that become increasingly difficult to modify with age. Between ages 4 and 6, amblyopia treatment can often restore normal or near-normal vision with appropriate intervention. This represents the optimal window when brain plasticity allows relatively easy reorganization of visual processing patterns.
Ages 7-9 represent a transitional period where treatment remains highly effective but requires more intensive approaches and longer duration. The visual system retains significant capacity for change, but therapeutic protocols must be more sophisticated and precisely calibrated to achieve optimal results.
After age 10, successful amblyopia treatment becomes increasingly challenging and time-intensive. While improvement remains possible through adolescence and even adulthood, the effort required increases dramatically, and outcomes become less predictable. Early intervention provides the best return on investment in terms of time, effort, and final visual function.
Real Timeline Comparisons by Age Group
Children ages 4-6 receiving professional vision therapy typically show measurable improvement within 4-6 weeks and achieve significant functional gains within 4-8 months. The visual system’s high plasticity allows rapid adaptation to new input patterns and the development of stable binocular vision skills.
Ages 7-9 require 8-12 months of intensive therapy for comparable results. Treatment protocols must address more entrenched suppression patterns and may need to overcome compensatory habits developed during previous months or years of poor binocular vision.
Children ages 10 and older often need 12-18 months of specialized protocols combining traditional vision therapy with newer techniques like perceptual learning. Success rates decrease, and outcomes may be limited compared to earlier interventions, though meaningful improvement remains achievable.
DIY game approaches typically show minimal lasting improvement regardless of age, often requiring 2+ years of consistent effort for changes that professional therapy achieves in months. The delay created by ineffective DIY attempts moves children from optimal treatment periods into more challenging age ranges.
Cook Vision Therapy’s Evidence-Based Game Integration Protocol
Professional vision therapy incorporates game elements strategically within comprehensive treatment protocols while addressing underlying visual dysfunction that games alone cannot correct. This integrated approach achieves lasting results by combining motivation benefits of games with the clinical precision of medical treatment.
The Cook Method: Four-Phase Integration System
Phase 1: Comprehensive Assessment and Foundation Building
Detailed evaluation identifies specific visual deficiencies that contribute to amblyopia beyond simple acuity reduction. Testing includes binocular vision assessment, eye movement evaluation, accommodation function analysis, and visual processing skills measurement. This comprehensive approach reveals multiple factors that games cannot address.
Phase 2: Strategic Game Integration with Clinical Oversight
Selected games are integrated once foundational skills reach minimum thresholds for safe progression. Game selection targets specific deficiencies identified during assessment rather than general amblyopia symptoms. Professional supervision ensures proper calibration and monitors for signs of visual stress or inappropriate compensation patterns.
Phase 3: Advanced 3D Vision Training and Real-World Application
Advanced techniques develop sophisticated binocular vision skills required for optimal function in daily activities. Stereogram training, random dot exercises, and fusion range expansion activities prepare the visual system for real-world demands beyond basic game scenarios.
Local Resources & Citations
Cobb County School District Vision Screening Guidelines
Official protocols for identifying vision problems in students, including referral criteria and accommodation procedures for children with visual impairments affecting academic performance.
Georgia Department of Public Health – Children’s Medical Services
State-funded vision screening programs and resources for families seeking specialized pediatric care, including eligibility requirements for vision therapy coverage.
Centers for Disease Control and Prevention – Vision Health Initiative
Research-based information about amblyopia prevalence, treatment effectiveness, and evidence-based therapeutic approaches for parents seeking authoritative medical guidance.
Kennesaw State University – College of Optometry Research
Academic research on vision therapy effectiveness and amblyopia treatment outcomes providing scientific context for treatment decisions and therapeutic approaches.
Your Next Steps: From Game Frustration to Vision Success in Marietta
Transition from ineffective DIY attempts to professional treatment requires specific steps that maximize the likelihood of successful outcomes while minimizing additional delay. This systematic approach addresses common concerns while providing clear direction for concerned parents.
Immediate Action Plan for Optimal Results
Step 1: Temporarily Discontinue Current Game Activities
Stop current vision games for 1-2 weeks before a professional assessment to allow the visual system to return to baseline function. Continued ineffective stimulation can mask underlying problems and interfere with accurate evaluation. This brief pause also reduces child frustration and resistance to future therapeutic activities.
Step 2: Document Previous Efforts and Current Struggles
Gather information about games tried, duration of use, any improvements noted, and specific difficulties encountered. Include academic concerns, sports participation challenges, and behavioral changes related to vision activities. This documentation helps professionals understand what approaches have failed and why.
Step 3: Schedule Comprehensive Professional Assessment
Contact Cook Vision Therapy within two weeks to schedule an evaluation while current struggles remain fresh and motivation for change remains high. Early appointment availability often exists for families transitioning from unsuccessful DIY attempts.
Step 4: Prepare the Child for Professional Evaluation Experience
Explain the upcoming assessment as “helping the eye doctor understand exactly how to help your eyes work better together.” Avoid references to previous game failures or medical necessity that might create anxiety. Emphasize that this evaluation is more comprehensive and personalized than previous approaches.
What Makes Cook Vision Therapy Different in Marietta
Cook Vision Therapy specializes exclusively in vision therapy and neuro-optometric rehabilitation, unlike general optometry practices that treat amblyopia as one of many conditions. This focused expertise translates to more sophisticated treatment protocols and better outcomes for complex cases.
Comprehensive approach addresses all aspects of functional vision beyond basic acuity improvement: depth perception, eye-hand coordination, visual processing speed, and sustained visual attention. This prevents the partial improvements typical of single-technique approaches.
Questions about your child’s specific situation? Speak directly with our vision therapy specialists who can provide immediate guidance based on 30+ years of serving Metro Atlanta families.
FAQs
-
Initial improvements (better eye contact, reduced squinting) appear within 2-4 weeks, but measurable vision acuity gains require 3-4 months of daily 30-45 minute sessions. After 8-12 weeks without measurable vision changes, the approach has likely reached its therapeutic ceiling. Professional evaluation becomes necessary when progress stalls to avoid wasting critical treatment time during peak brain plasticity periods



